Osteoarthritis Affects Millions. Why Are So Many People Still Afraid to Move?
May 12, 2026
May is Osteoarthritis Awareness Month, a time to bring attention to one of the most common and misunderstood chronic conditions in the world.
More than 528 million people worldwide were living with osteoarthritis in 2019, a 113% increase since 1990. (WHO) In the United States alone, about 33 million adults have osteoarthritis. (CDC)

Despite how common it is, many people still leave an osteoarthritis diagnosis feeling confused, discouraged, or afraid to move.
That fear makes sense.
Pain changes how people think about their bodies. If walking hurts, it is natural to wonder whether damage is being done. If a knee feels stiff after activity, many people assume they should rest more. Terms like “bone-on-bone,” “degeneration,” or “wear and tear” can make movement sound risky, even though physical activity is among the most recommended treatments for osteoarthritis.
Over time, people may start avoiding activities they once enjoyed. Walking less. Exercising less. Turning down trips, hobbies, or social activities because movement feels uncertain.
For many people with osteoarthritis, the challenge is not just pain itself. It is what the pain starts to mean.
Osteoarthritis is common, but it is not simply “just aging.”
Osteoarthritis is the most common form of arthritis and a leading cause of disability worldwide. It can affect the knees, hips, hands, spine, and other joints, leading to pain, stiffness, swelling, and difficulty with daily activities.
It becomes more common with age, but osteoarthritis is not simply an inevitable part of getting older. The World Health Organization notes that while age is a risk factor, osteoarthritis is not an unavoidable consequence of aging.
That is important because the way people understand osteoarthritis can shape how they respond to it.
When someone believes their joints are fragile or “worn out,” movement may begin to feel dangerous. Some people start waiting for pain to fully disappear before becoming active again. Others stop exercising altogether because they are worried they are making things worse.
But avoiding movement entirely can create its own problems over time. Less activity may lead to more stiffness, reduced strength, lower confidence, and a growing sense that the body cannot handle movement anymore.
Why staying active with osteoarthritis can feel so difficult
People with osteoarthritis are often told to exercise more. But research shows that staying active is not always straightforward.
A systematic review published in BMJ Open examined barriers to physical activity in people with hip and knee osteoarthritis. Researchers found that barriers extended far beyond pain itself. They included uncertainty about what activities were safe, previous negative experiences with exercise, distress, lack of support, low confidence, and beliefs about osteoarthritis and movement.
In other words, many people are not simply deciding whether or not to exercise. They are trying to interpret symptoms, make sense of conflicting advice, and figure out what their pain means.
This is one reason osteoarthritis can become such a frustrating cycle. Pain may lead to less movement, less movement may reduce strength and confidence, and everyday activities can start to feel harder over time.
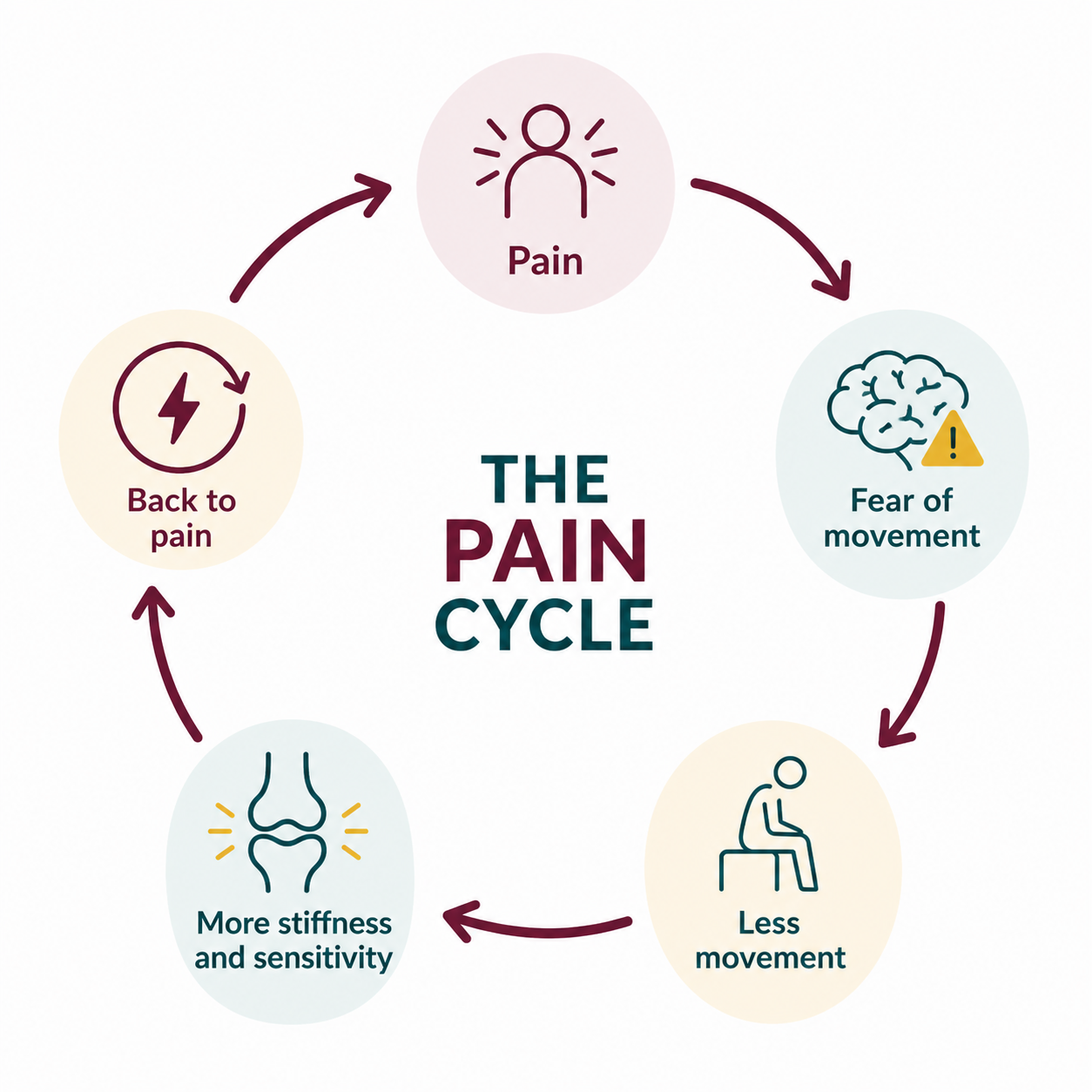
We discussed this cycle further in our previous article on osteoarthritis pain and the pain cycle.
Movement does not have to look perfect to matter
One of the biggest misconceptions about physical activity is that it only “counts” if it looks like a structured workout.
For many people with osteoarthritis, movement may begin much smaller than that.
A short walk around the block. Standing up more often during the day. Gentle strengthening exercises. Stretching while watching TV. Gardening. Dancing in the kitchen. Taking the stairs when it feels manageable.
Research consistently supports physical activity as an important part of osteoarthritis management, but that does not mean people need to become marathon runners or push through severe pain.
Often, the goal is simply to help movement feel more approachable, more sustainable, and less intimidating.
At Rethink OA, we often come back to a simple idea:
Every step counts.
Not because one walk fixes osteoarthritis, but because small experiences of movement can help people reconnect with activities, routines, and parts of life that pain may have interrupted.
Awareness should include better support and better information
Osteoarthritis Awareness Month should be about more than statistics.
It should also be about improving the way people understand osteoarthritis and helping them feel more supported in managing it.
People deserve clear, evidence-based information. They deserve guidance that goes beyond “just lose weight” or “just exercise.” They deserve care that recognizes both the physical and psychological challenges that can come with persistent pain.
In our randomized clinical trial of Rethinking Osteoarthritis, 408 people with knee osteoarthritis participated in a digital program designed to improve understanding of osteoarthritis, pain, movement, and mindset. Compared with no intervention, participants who completed Rethink OA increased physical activity and improved outcomes, including fear of movement, self-efficacy, perceived need for surgery, and physical and mental health. The biggest shift wasn't forcing more exercise. When people changed how they thought about osteoarthritis and movement, they moved more on their own.
Mindset is not a cure for osteoarthritis. But research increasingly suggests that the way people understand pain and movement can influence how active, confident, and capable they feel in daily life.

Helpful Osteoarthritis Resources
If you are looking for additional information or support during Osteoarthritis Awareness Month, these organizations provide trustworthy, evidence-based resources:
FAQ
Is walking good for osteoarthritis?
For many people, walking can be a helpful low-impact activity that supports joint health, strength, and overall function. The right amount varies from person to person, and starting gradually is often helpful.
Does exercise wear out arthritic joints?
Research does not support the idea that appropriate physical activity “wears out” joints. In fact, exercise is consistently recommended in osteoarthritis treatment guidelines because it can improve strength, function, and quality of life.
Why does my osteoarthritis pain change from day to day?
Osteoarthritis symptoms can be influenced by many factors, including activity levels, sleep, stress, inflammation, sensitivity, and overall health. More pain does not always mean more damage is occurring.
Can osteoarthritis get better?
While osteoarthritis itself does not fully reverse, many people can improve pain, physical function, strength, confidence, and overall quality of life with the right support and management strategies.
Should I avoid movement during an osteoarthritis flare-up?
Sometimes movement needs to be modified during a flare-up, but complete rest is not always the answer. Gentle movement and gradual return to activity are often recommended depending on symptoms and guidance from a healthcare professional.
What kinds of exercise are best for osteoarthritis?
Walking, strengthening exercises, cycling, swimming, stretching, and other low-impact activities are commonly recommended. The best type of movement is often the one that feels manageable and sustainable for you.
Can mindset really affect osteoarthritis symptoms?
Pain is real and osteoarthritis is a physical condition. At the same time, research suggests that beliefs, expectations, fear, stress, and confidence can influence how people experience pain and engage with movement and daily activities.
About the Author
Melissa Boswell, PhD, is a bioengineer and digital health founder with nearly a decade of experience working in osteoarthritis, movement science, and human performance. She is the founder of Rethink OA, a clinically validated digital program developed from research conducted with collaborators at Stanford University and published in npj Digital Medicine. Her work focuses on helping people better understand pain, movement, and behavior change in osteoarthritis.

Move More. Fear Pain Less.
Learn how to reduce pain, stay active, and support your joints—starting today.

